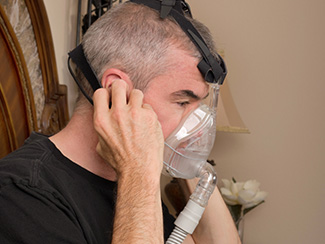
Respiratory muscle weakness is a common feature of motor neurone disease (MND). It can affect breathing, sleep and overall health.
Changes may develop gradually and can be difficult to recognise in the early stages. Early identification and timely support can help manage symptoms, reduce complications and improve quality of life.
On this page you will find:
- how respiratory symptoms may present
- how they may affect day to day life
- what to consider in practice
- respiratory support options
- further guidance and resources.
Understanding respiratory symptoms in MND
Respiratory symptoms in MND are caused by weakness of the muscles used for breathing.
This can lead to:
- reduced lung ventilation
- difficulty clearing secretions
- changes in breathing during sleep.
Symptoms often develop gradually and may not be immediately recognised.
How this may present in practice
Early symptoms may be subtle and are often worse at night.
You may notice:
- breathlessness, particularly on exertion or when lying flat
- disturbed sleep or frequent waking
- morning headaches
- daytime sleepiness or fatigue
- difficulty concentrating
- a weak cough or difficulty clearing secretions.
Family members or carers may notice changes before the person themselves.
What to consider in practice
Early recognition and referral are important.
- consider respiratory involvement in people with MND, even if symptoms are mild
- refer to specialist respiratory services for assessment
- involve the multidisciplinary team, including neurology and specialist nurses
- monitor for changes in symptoms over time
- consider the impact on sleep, fatigue and daily function.
Discuss changes with the person and those close to them, and review regularly as needs change.
Respiratory support
A range of approaches may be used to support breathing and manage symptoms.
Non-invasive ventilation (NIV)
NIV is commonly used to support breathing in MND. It can improve symptoms, sleep quality and quality of life.
Airway clearance and secretion management
Support may include techniques or equipment to help clear secretions.
Tracheostomy ventilation
In some cases, tracheostomy ventilation may be considered. This is a more complex intervention and involves significant practical, clinical and personal considerations. Decisions should be made with the person, their family, and the multidisciplinary team, taking into account individual preferences and goals of care.
Warning: Oxygen therapy
Oxygen should be used with extreme caution in MND. Respiratory symptoms are usually caused by reduced ventilation rather than low oxygen levels, and oxygen alone may worsen carbon dioxide retention. Specialist advice should be sought before initiating oxygen therapy.
Other considerations:
- support with positioning
- managing fatigue and energy levels
- advance care planning and future discussions.
Decisions about respiratory support should be guided by the person’s preferences, clinical need and overall goals of care.
Further guidance and resources
You may find the following resources helpful:
Breathing and ventilation information for people with MND
NIV4MND (SITraN): an online toolkit supporting respiratory management in MND, with a focus on NIV
MyBreathing (SITraN): an educational website for people with MND, providing information on breathing support and NIV.
You can find further guidance on symptom management and support across the Management of MND section.
Page last updated: April 2026
Next review: April 2029