NHS Continuing Healthcare (CHC) provides a package of care NHS and specialist equipment funded by the NHS. The funding provided is not means tested and is free at the point of access.
The CHC assessment can be complex and can take a while to complete. Understanding how the system works, and what makes someone eligible for CHC can make the process smoother, both for people with MND and the professionals supporting them. If a person qualifies for CHC it can make a big difference to their care and quality of life.
To qualify for CHC, the person must be assessed as having a ‘primary health need’. This usually means they have nursing or healthcare needs which cannot be met by adult social care services, such as:
- complex needs which require a high level of skill to manage
- a need for ongoing care
- a condition which is changing quickly and causing concerns in managing care.
Note: If the person’s condition is deteriorating rapidly, or you suspect they are nearing the end of their life, a doctor or a registered health professional should complete the Fast Track Pathway Tool. See heading below.
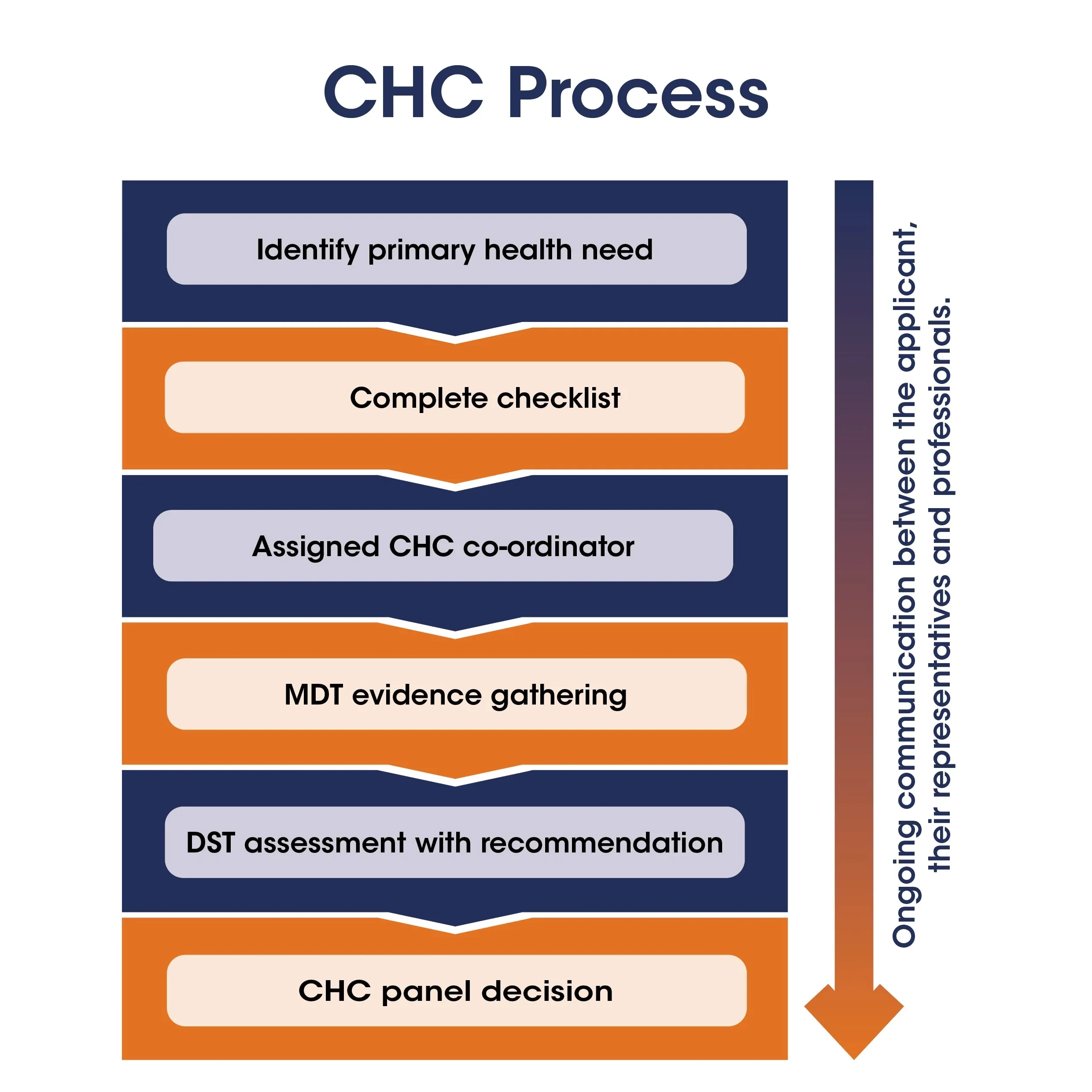
CHC process flow chart
Below is a flow chart outlining the steps involved in accessing NHS Continuing Healthcare. The drop down menus below go into further details.
Where is CHC available?
England
CHC funding is available to people across England. In order to access NHS Continuing Care in England any person who may be eligible will be referred for a full assessment following the application of a screening process. The assessment decision is ratified by local Integrated Care Boards who will arrange a package of care.
Wales
Many of the CHC rules in England also apply in Wales. Wales has its own CHC framework, Continuing NHS Health Care. The process is similar to that in England, however, the Local Health Board ratify the decision and commission a package of care for a person who meets the eligibility criteria following assessment. Contact Health in Wales (NHS Wales) for more information.
Northern Ireland
In Northern Ireland, there is no explicit framework currently on NHS CHC provision. Services are based on an integrated system for the delivery of health and social services. In Northern Ireland services often follow NHS guidance, so a similar package of care may be offered. NHS Continuing Healthcare may be available in some cases, however, there is no detail as to how Health and Social Care Trust staff should determine eligibility for this service other than through a ‘comprehensive assessment of need’. More information can be provided by the six Northern Irish local Health and Social Care Trusts. Contact your local health and social care trust for advice.
Scotland
In Scotland, the provision of health and social care services is the joint responsibility of Local Authorities and Health Boards through an integrated system of delivery. NHS Continuing Healthcare is available in Scotland to those individuals who are assessed as eligible to receive this service. Eligibility is determined using guidance issued by the Scottish Government entitled Hospital Based Complex Clinical Care | Care Information Scotland.
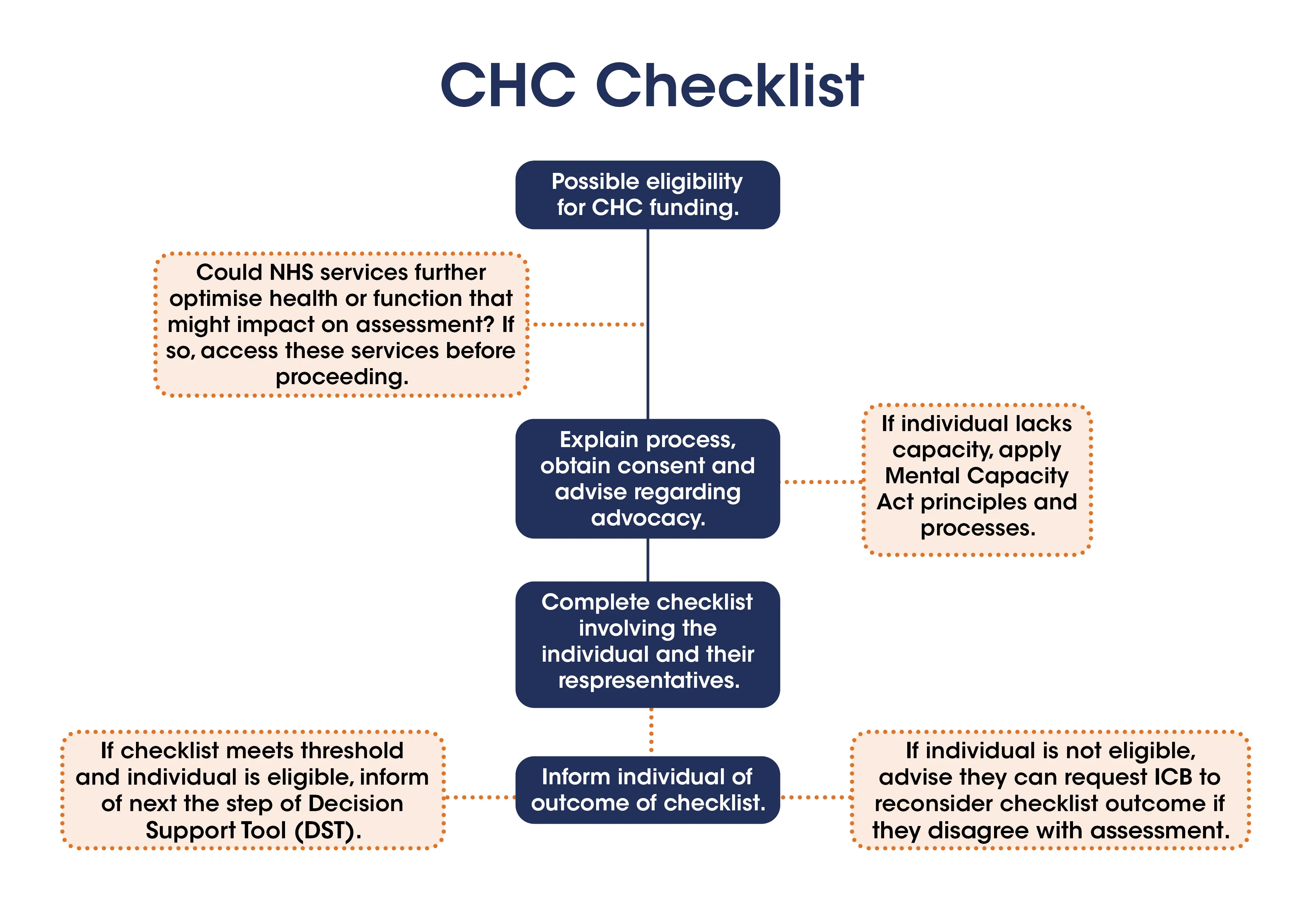
Stage 1: NHS continuing healthcare checklist
An application for CHC is usually done in two stages. The first is a checklist completed by a health or social care professional, used to decide if a full assessment is needed. The person with MND should be told in advance that the checklist is to be completed, and they should be included in the process. They may choose to have an advocate, family member or someone involved in their care with them when the checklist is completed.
The checklist looks at the person’s needs using 11 headings, known as domains. They are:
- breathing
- nutrition
- continence
- skin
- mobility
- communication
- psychological and emotional needs
- cognition (thinking and reasoning)
- behaviour
- drug therapies and medication
- altered state of consciousness.
Needs will be scored in each domain as either high, moderate or low.
If the person gets an overall high score, they will need the full assessment.
View NHS checklist guidance and forms
The flow chart below shows the steps involved in the checkilist stage of the assessment.
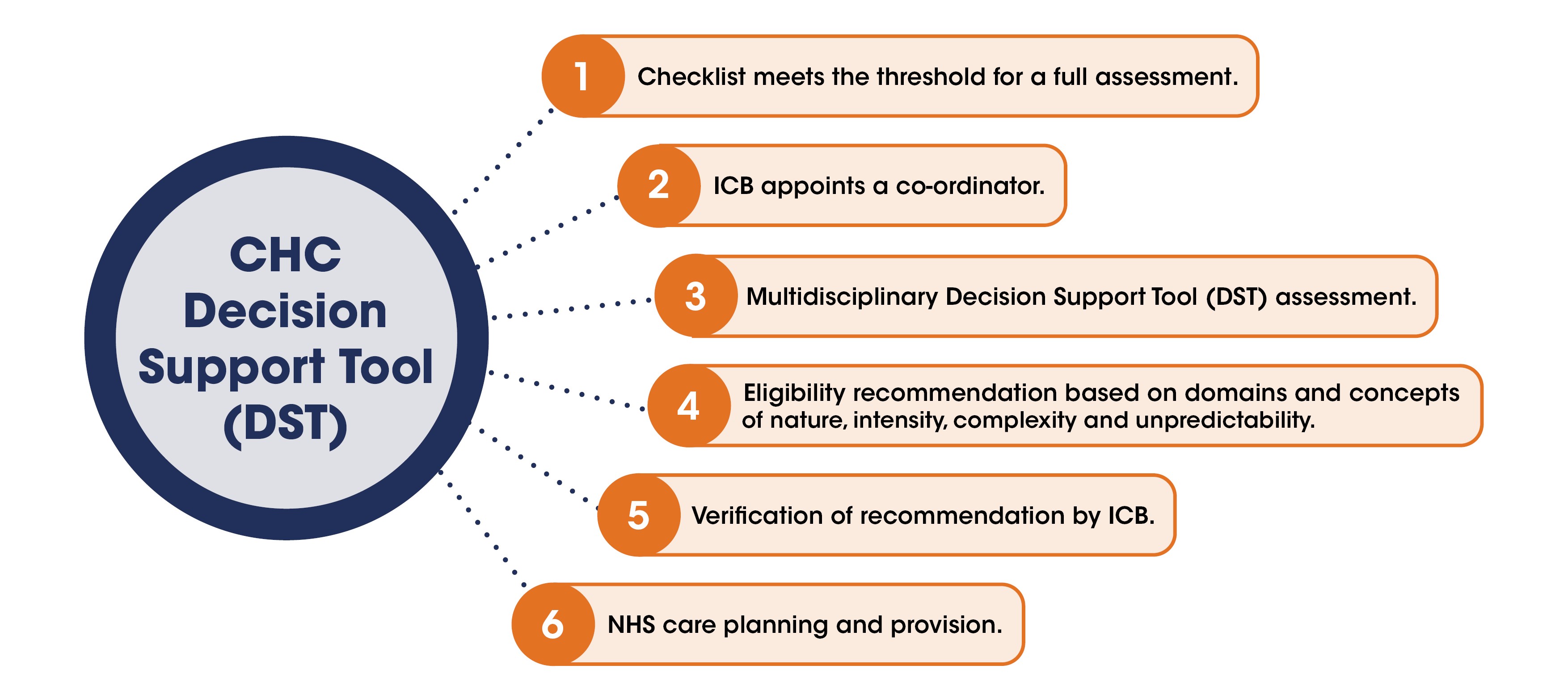
Stage 2: NHS continuing healthcare decision support tool
The full assessment is a detailed review of the person’s health and social care needs using the Decision Support Tool (DST). The assessment should involve a range of professionals involved in the person’s care, who knows them well.
If members of the health and social care team cannot be at the assessment, the CHC assessors should ask for detailed information to help them understand the person’s needs. The person with MND’s own views about their health should also be recorded. They may find it helpful to have an advocate, family member or friend with them.
Assessment using the DST is not based on any particular diagnosis. It will focus on the nature, intensity, complexity and unpredictability of the person’s individual needs.
The assessment follows the 11 domains in the checklist, plus another for ‘any other significant needs’.
View our information sheet for professionals for details of how symptoms of MND may fit the domains
It is essential that professionals and the person with MND give as much detail as possible during the assessment, including:
- symptoms that are being well managed
- details about symptoms on bad days, as well as good days.
In each domain of the DST, needs are scored from "no needs" up to "priority" needs. The person should qualify for CHC if they have:
- a priority level need in the breathing, behaviour, drugs and medications or altered state of consciousness domains
- two domains scored as severe.
Other combinations of scores may also qualify, but scoring mostly ‘no needs’ or ‘low needs’ would mean the person is unlikely to qualify.
At the end of the assessment, the health professionals will make a recommendation about whether the person qualifies for CHC.
View NHS DST guidance and forms
The chart below shows the stages involved in the DST stage of the CHC assessment.
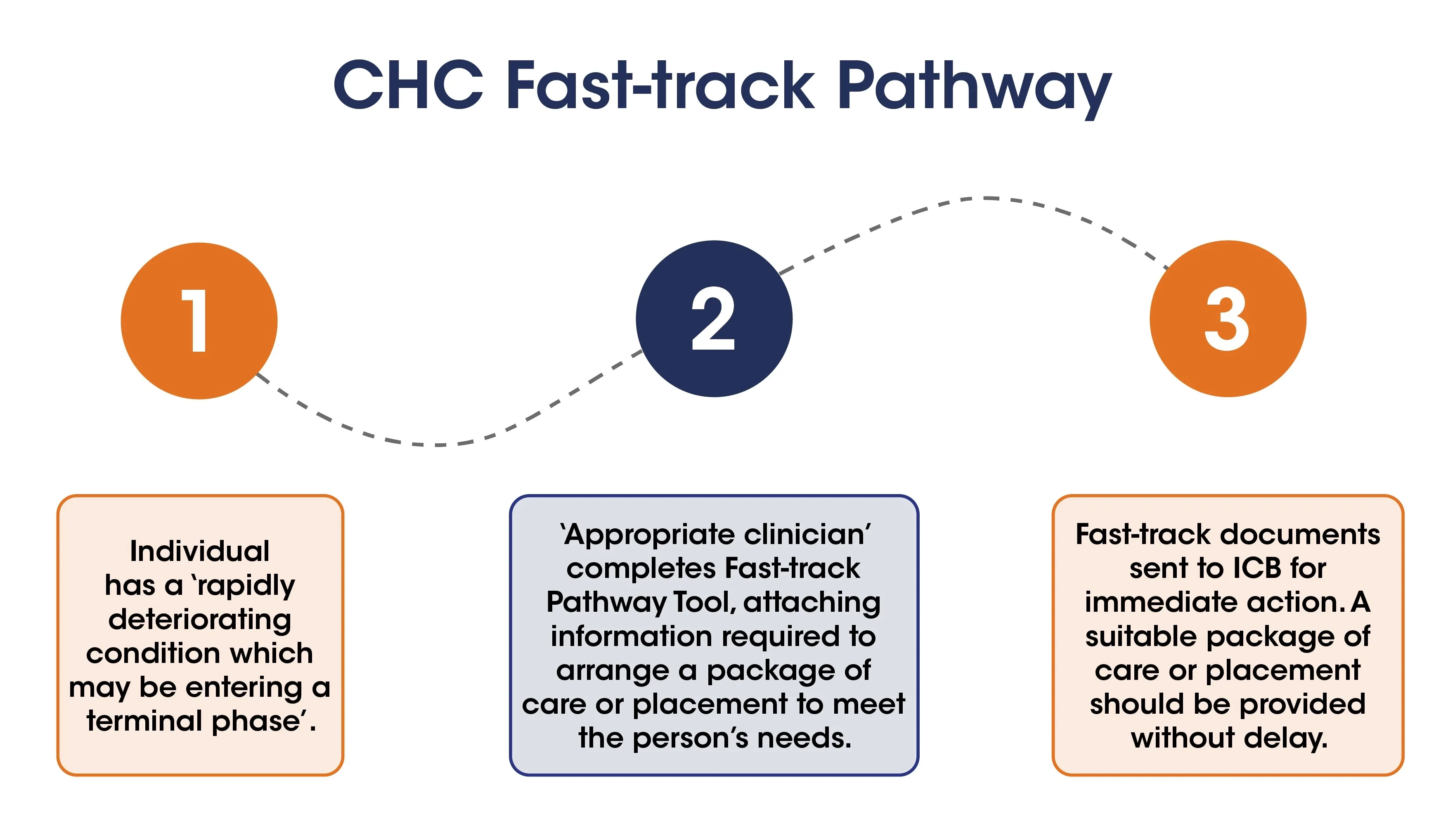
Fast-track applications
If the person's condition is getting worse very quickly and the health and social care team feel they may be reaching the end of life, they may complete the Fast-track Pathway Tool. This must be completed by a doctor or a registered health professional.
Using the fast track route, people should be accepted for CHC funding without delay. It is important to give enough detail, so the referral should be made by a professional who knows the person well and has good understanding of their needs.
View NHS fast-track guidance and forms
The chart below shows the stages of a CHC fast-track application.
Appeals
If an application for CHC is refused, the person should receive a written response telling you why, with details of how to appeal against the decision.
If they disagree with the outcome of the CHC assessment, they can appeal and send any evidence they feel was missed.
If they are unhappy with the outcome of the appeal, they can ask for an independent panel review. This must be done within six months.
Let's talk CHC - peer support group
Our CHC peer support group meets every six weeks on Zoom. It is open to people with or affected by MND, Association volunteers and health and social care professionals who want to find out more about the process of obtaining CHC, or are facing problems with an existing care package.
The group is facilitated by volunteers. For further details and joining instructions for the meetings, please email chc@mndassociation.org
CHC direct referral pilot
We are launching a Continuing Healthcare (CHC) direct referral pilot in partnership with Beacon CHC Independent Advocacy Service on 1st April 2025.
Direct referrals will be made to Beacon, via our MND Connect Helpline. This service provides 90 minutes of free, personalised advocacy support for all aspects of CHC. The pilot, which is set to run for an initial six-month period, will be evaluated regularly.
Please continue to signpost to or access the MND Connect Helpline in the first instance on 0808 802 6262, or email mndconnect@mndassociation.org, for any CHC issues.
Useful resources
From the MND Association
- What is NHS Continuing Healthcare? animation gives a simple overview of the CHC process.
- CHC and MND webinar recording - presented by Hayley Koumas, CHC Improvement Co-ordinator at the MND Association.
- Information sheet P7 - NHS Continuing Healthcare for MND for health and social care professionals goes through all the domains in the CHC assessment and describes how MND may fit within these.
- Information sheet 10D - NHS Continuing Healthcare for people with MND lays out the process in detail, with useful links to further information and support.
- MND Matters podcast episode 20 - NHS Continuing Healthcare features Dan Harbour from Beacon CHC, Dave Setters, who is living with MND and Marian Ward, whose husband had MND, discussing the application process for CHC, and sharing some tips for those going through the assessment process.
- Campaigns webpage on CHC includes updates on the work we are doing to influence the government and NHS to improve the CHC system.
External resources
- National framework for NHS continuing healthcare and NHS-funded nursing care guidance sets out the principles and processes of the national framework for NHS continuing healthcare and NHS-funded nursing care.
- Beacon CHC offer a helpline and resources to support people going through the CHC process. Their Information and Advice Service offers general advice and the opportunity to book a consultation of up to 90 minutes of free advice with a specialist adviser.
- NHS continuing healthcare, social care, and support guide gives an overview of CHC for people going through the process.
- Personal health budgets in NHS Continuing Healthcare (CHC) information from NHS England includes information and videos about how personal budgets can support people receiving CHC.